How Long Does Ativan Stay in Your System?
Ativan is one of the brand names for the benzodiazepine drug lorazepam. Lorazepam is a benzodiazepine drug that is most commonly prescribed for the treatment of clinically significant issues with anxiety and as an anesthetic or preanesthetic, but it may also be useful in treating seizures, as an aid for sleep, and in the treatment of withdrawal symptoms from alcohol or other benzodiazepines.
Use of Benzodiazepines

Benzodiazepines are one of the most prescribed groups of medicines in the United States. According to estimates released by the Substance Abuse and Mental Health Services Administration (SAMHSA), approximately 7.3 million people admitted to using lorazepam products at least once during 2016.
Benzodiazepines were developed as alternatives to the addictive barbiturates that were once widely prescribed for the treatment of anxiety and for seizure control. The overprescription of barbiturates led to numerous substance abuse issues and well-publicized overdoses. The famous singer and actress Judy Garland overdosed on barbiturates and passed away as a result. It was hoped that benzodiazepines would have less potential for abuse; however, these drugs are also widely abused. For instance, according to the data provided by SAMHSA, 786,000 individuals admitted to at least one misuse of lorazepam in 2016.
All of the benzodiazepines are designated as controlled substances by the Drug Enforcement Administration (DEA), and most of them are listed in the Schedule IV (C IV) categorization. This means that these drugs have a moderate potential to be abused and may result in physical dependence if they are used consistently.
Using benzodiazepines for the treatment of anxiety or as a sleep aid should not be a long-term solution to the problem. Instead, benzodiazepines should be used to help individuals cope with their anxiety or issues with sleep while they learn behavioral methods to control their situation (e.g., with various types of psychotherapy or other interventions). Using benzodiazepines to address common issues with normal nervousness and frustration is a potential misuse of the medication.
Physicians should not prescribe benzodiazepines to address issues with anxiety unless the individual has a specific mental health disorder or some other neurological condition that results in clinically significant anxiety. The continued use of benzodiazepines as sleep aids can foster abuse because individuals will typically develop tolerance rapidly and require more of the drug to produce the effects they seek. This can lead to issues with misuse and abuse.
All benzodiazepines are considered to be minor tranquilizers or central nervous system depressant drugs, and they are sometimes listed as sedative drugs. Benzodiazepines all have a similar chemical structure and affect the neurotransmitter gamma-aminobutyric acid (GABA). Neurotransmitters are chemicals used by the nerve cells in the brain (neurons) to communicate with each other and to initiate the vast majority of human actions. GABA is an inhibitory neurotransmitter, meaning that when it is released, it slows down the functioning of other neurons in the brain. This accounts for its ability to address issues with anxiety, act as a sleep aid, and treat seizures.
There are risks to long-term use of benzodiazepines, such as the development of physical dependence. Long-term use of Ativan and other benzodiazepines carries the risk of significant potential side effects that can include issues with memory and the possible development of dementia in elderly individuals. Benzodiazepines like Ativan are also potentially fatal when combined with other central nervous system depressants, such as alcohol, other benzodiazepines, and opiate drugs.
Ativan Effect Timeline

When taken orally, Ativan is absorbed slowly and considered to have an intermediate action of onset (between 15 and 30 minutes for most people) compared to other benzodiazepines. An oral dose of Ativan will reach its peak effects within about two hours for most individuals.
Ativan Half-Life & Elimination
The half-life of Ativan, the amount of time it takes an individual’s system to metabolize the drug to half its original concentration in the bloodstream, is often stated to be about 12 hours; however, a better estimate is between 10 and 20 hours for most individuals. In most cases, it takes about five to six half-lives for the medicinal dose of a drug to be eliminated from an individual’s system. Abusers with significant tolerance may take amounts that are extremely high, and it might take longer for the drug to be eliminated.
Research indicates that the majority of the drug is metabolized in the liver and then eliminated through the kidneys (through urine). For most individuals, the majority of Ativan is eliminated within five days of taking it; however, there are some metabolites of lorazepam (substances that are produced as a result of breaking down the drug) that may remain in a person’s system for longer than a week.
How Long Does Ativan Remain in the Body?
 Depending on the situation, individuals being tested for drug use may not be screened for benzodiazepines. Many of the traditional drug screens (e.g., SAMHSA 5 Panel Test) may not screen for benzodiazepines, whereas more extensive screens (e.g., SAMHSA 10 Panel Test) will detect them.
Depending on the situation, individuals being tested for drug use may not be screened for benzodiazepines. Many of the traditional drug screens (e.g., SAMHSA 5 Panel Test) may not screen for benzodiazepines, whereas more extensive screens (e.g., SAMHSA 10 Panel Test) will detect them.
Based on the available research, there are estimated detection windows for how long Ativan will show up on a drug test.
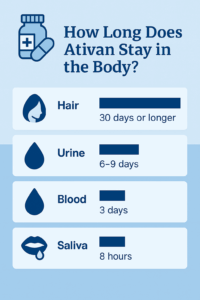
- Lorazepam may be detectable in urine samples for up to six days, and some of the metabolites may be detectable for even longer (nine days). If regularly abused, urinalysis may reveal the presence of lorazepam after a week or longer.
- Research indicates that blood samples may be able to reveal the presence of lorazepam for up to three days.
- Hair samples may be able to detect the presence of lorazepam for 30 days or longer after ingestion. Typically, the drug will not test positive in a hair sample until several days after the person is taken it.
- The use of saliva tests may reveal the presence of Ativan for up to eight hours after use.
The most common method to test for the presence of Ativan is urinalysis. Blood tests are considered too invasive, and hair samples are typically considered to be too expensive in most cases.
Factors That Can Influence How Long the Drug Stays in the Body
There are several factors that can influence the detection time for any drug, including Ativan.
- Individual differences in metabolism, kidney functioning, and health can affect how any drug is metabolized and eliminated from the body. Individuals with kidney or health issues will most likely metabolize and eliminate the drug more slowly.
- Older individuals will typically have slower metabolisms and thus eliminate drugs slower than younger individuals.
- Heavier individuals appear to eliminate lorazepam quicker than lighter individuals, so bodyweight may also play a factor in some cases.
- The frequency and amount of the drug taken will affect how long the drug remains in the system. Individuals who chronically use the drug at regular intervals or take high amounts of the drug will eliminate the drug more slowly than individuals who have not developed significant tolerance.
- Using lorazepam with other drugs can affect the elimination time of the drug. The classic example is alcohol, which is metabolized first by the liver. Other combinations of drugs can also slow down the elimination rate of Ativan, such as other benzodiazepines or stimulants.
- Hydration may have a minor effect on how quickly Ativan is eliminated from the system. Individuals who are well hydrated may eliminate the drug at a faster rate than those who are not.
- In some instances, certain foods could affect the elimination rate of any drug in the system. Eating fatty foods before or while using the drug is often thought to slow down the elimination of many drugs and other substances from the system.
